Making the Screw-in Prosthesis Installation System Safer
Emil LA Svoboda, DDS, PhD, FAAID, DABOI/ID
Presented at the AAID Southern District Meeting “Generating Implant Longevity: Engineering Excellence” and annotated for web viewing.
 Making the Screw-in Prosthesis Installation System Safer
Making the Screw-in Prosthesis Installation System Safer
Emil LA Svoboda, DDS, PhD, FAAID, DABOI/ID
Presented at the AAID Southern District Meeting “Generating Implant Longevity: Engineering Excellence” and annotated for web viewing.
Abstract: There is a growing concern regarding the mechanical and biological failure of dental implants and their attached prosthetics.
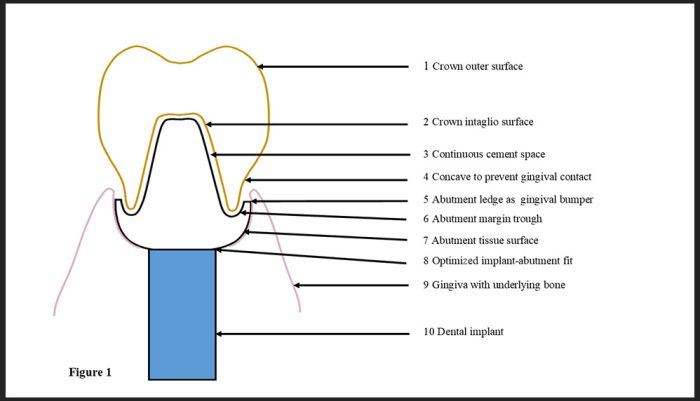
Identifying the root causes of treatment complications is essential to mitigating their harmful effects. The root causes of treatment complications are primarily mechanical and, fortunately, under the control of dentists. Dr. Svoboda proposes that implant manufacturers and sellers should provide dentists with relevant technical information regarding the fit-tolerances of their implants and connecting parts so dentists have some rational means of purchasing the best products for their patients. Manufacturers must also provide dentists with installation instructions that include their inherent risk factors for complications and that their CAD/CAM-related products give dentists more control over efficiently customizable features that can make treatment safer for patients. Unfortunately, current features embed legacy prosthetic designs that are known to expose patients to several known risk factors for peri-implant disease and treatment failure. The author demonstrates how following two rules can make legacy installation systems safer and how the Reverse Margin System can also make treatment more straightforward for the dentist.
I welcome all your questions and comments. I hope this “Implant Essentials: The BIG Questions” segment of this journal will help guide you to a better understanding of your craft, so you can do the best possible job for your patients. Besides, it would probably give you more pleasure basking in the glory of success, rather than trying to manage disappointed patients with complications…..
Making the Screw-in Prosthesis Installation System Safer
Abstract: There is a growing concern regarding the
13 May, 20241015 DownloadsWhy and When does Splinting Crowns and Bridges make Treatment Better for Patients
Abstract: In Spectrum Implants October 2022 I intr
03 February, 2023893 DownloadsThe Reverse Margin System and Supporting Concepts Designed to Make Implant Treatment Better
Abstract: The Reverse Margin System (RMS) d
02 January, 20231020 DownloadsMaking Fixed Prosthesis Installation Safer by Preventing Several Risk factors for Peri-implant Disease
Abstract: There continues to be much dialogue abou
07 December, 2022603 DownloadsDo Dental Implants Fail 10 Times More than Natural Teeth? A Critical Review and Related Commentary
Overly grandiose and poorly substantiated titles r
18 October, 2022757 DownloadsDo dentists receive the support they need from educators, dental laboratories, implant manufacturers, implant sellers, and Government regulators to enable them to do a better job for their patients?
Abstract: This article reveals the perspective of
14 October, 2022534 DownloadsSafer Intraoral Cementation is the Gold Standard for Fixed Prostheses Installation
Abstract: This slide presentation is a concise ove
08 June, 2022661 DownloadsScrewmentation The Svoboda Way
Abstract: What prompted the development of the pro
02 June, 2022649 DownloadsEffect of Margin Design, its Subgingival Depth and Installation Pressure on Subgingival Cement and Open Margins: an in vitro study
Emil LA Svoboda PhD, DDS, Anit Sharma DDS a
23 May, 2022665 DownloadsThe Big Question with Emil Svoboda PHD DDS
I welcome all your questions and comments. I hope
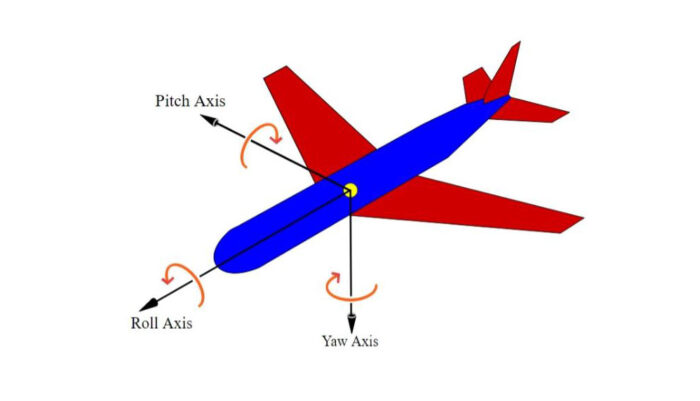
25 April, 2022627 DownloadsFixed Prosthesis Installation: An Aviation Analogy Considering 3-D Position, Yaw, Pitch and Roll
Citation: Svoboda E.L.A. Fixed Prosthetics: Positi
26 October, 20212553 DownloadsNew Dental Implant Terminology for Exposing and Mitigating the Root Causes of Installation Related Treatment Complications
As knowledge about dental implant treatment increa
25 August, 20211611 DownloadsExploring the BIG QUESTIONS about Implant Dentistry
Welcome to my new feature, Exploring the BIG QUEST
23 August, 20211558 DownloadsThe Screw versus Cement Debate: Will that be Peri-implant Disease by Misfits and Poor Access to Care or Bad Margins and Subgingival Cement?
Will that be Peri-implant Disease by Misfits and P
23 August, 2021756 DownloadsComparing the Chamfer and Reverse Margin System at Preventing Submarginal Cement
Emil LA Svoboda PHD, DDS. Anit Sharma DDS, Majid Z
16 June, 20211204 DownloadsMisfit implant parts and poor margins are the Standard of Care for implant prosthetics. Is anyone conflicted about this?
Citation: Svoboda Emil LA. Misfit implant parts an
10 May, 20211169 DownloadsAll-On-X A New Standard of Care
Citation: Svoboda Emil LA. All-On-X A New Standard
01 May, 2021928 DownloadsSafer Implant Treatment: Mitigating the Root Causes of Complications Related to Current Prostheses Installation Techniques Dr. Emil Svoboda
Citation: Svoboda ELA. Safer Implant Treatment: Mi
19 April, 20211327 DownloadsDental Implant Prosthetics: Achieving Retrievability and Reducing Treatment Complications by using a Modified Installation Technique Dr. Emil Svoboda
Citation: Dental Implant Prosthetics: Achieving Re
10 April, 20212088 DownloadsControlling excess cement during the process of intra-oral prosthesis cementation. Overcoming the Gingival Effects. Dr. Emil Svoboda
Citation: Controlling Excess Cement During The Pro
05 April, 20211715 DownloadsGovernment Quality Safer Prosthesis Installation Dr. Emil Svoboda
Citation: Svoboda ELA. Government Quality Manageme
01 April, 20213026 DownloadsPreventing Peri-implant Disease by Safer Prosthesis Installation: Managing the Macrogap and Residual Subgingival Cement
Dental implants are used in dentistry as tooth roo
25 March, 20211648 DownloadsEffectiveness of Implant Therapy Analyzed in a Swedish Population: Prevalence of Peri-implantitis – EDITORIAL by Emil L.A. Svoboda
Citation: Effectiveness of Implant Therapy Analyze
19 March, 20211593 DownloadsPreventing peri-implantitis by safer prosthesis installation Updated PDF
Svoboda Emil LA. Preventing Peri-Implantitis by Sa
15 March, 20211393 DownloadsSafer Intra-Oral Cementation: Prevention of Cement Voids under the Prosthesis Dr. Emil Svoboda
Citation: Safer Intra-Oral Cementation: Prevention
15 February, 20211822 DownloadsProsthesis Installation Technique using the Reverse Margin Design Principals
Citation: Prosthesis Installation Technique using
04 November, 20203965 DownloadsYou Want to Continue to Use Stock Abutments because they are Cheap? They Cause Expensive Preventable Complications Dr. Emil Svoboda
Citation: Svoboda Emil LA. So, You Want to Continu
12 August, 20191086 DownloadsTaming the Old Dragons of Dental Implant Prosthetics Dr. Emil Svoboda
Citation: Svoboda Emil LA. Taming the OLD Dragons
05 June, 20191031 DownloadsVDDS Preventing Peri-Implant Disease Dr. Emil Svoboda
Svoboda ELA. Preventing Complications Related to I
19 November, 20181318 DownloadsPrevention and Treatment of Peri-implant Disease Dr. Emil Svoboda
Introduction: Treatment involving dental implants
06 June, 20181622 DownloadsScrew versus Cement for Implant Prosthesis Installation. Part 2: The Game Changer the Tips the Balance to Favour Intra-oral Cementation
Part 2 [slideshare [slideshare id=56838352&
02 January, 2016Screw Vs Cement for Dental Implant Prosthesis Installation Part 1: The Logic Behind the Argument Dr. Emil Svoboda
Part 1 Screw Vs Cement for Dental Implant P
02 January, 2016The Evolution from Stock to Custom Abutments Allows for a Better Prosthesis Design that can Control the Gingival Effects and thus the flow of Excess Cement Dr. Emil Svoboda
Citation: The Evolution from Stock to Custom Abutm
13 September, 20151651 Downloads
Why and When does Splinting Crowns and Bridges make Treatment Better for Patients
Abstract: In Spectrum Implants October 2022 I intr
03 February, 2023893 DownloadsThe Reverse Margin System and Supporting Concepts Designed to Make Implant Treatment Better
Abstract: The Reverse Margin System (RMS) d
02 January, 20231020 DownloadsDo dentists receive the support they need from educators, dental laboratories, implant manufacturers, implant sellers, and Government regulators to enable them to do a better job for their patients?
Abstract: This article reveals the perspective of
14 October, 2022534 DownloadsScrewmentation The Svoboda Way
Abstract: What prompted the development of the pro
02 June, 2022649 DownloadsEffect of Margin Design, its Subgingival Depth and Installation Pressure on Subgingival Cement and Open Margins: an in vitro study
Emil LA Svoboda PhD, DDS, Anit Sharma DDS a
23 May, 2022665 DownloadsThe Big Question with Emil Svoboda PHD DDS
I welcome all your questions and comments. I hope
25 April, 2022627 DownloadsFixed Prosthesis Installation: An Aviation Analogy Considering 3-D Position, Yaw, Pitch and Roll
Citation: Svoboda E.L.A. Fixed Prosthetics: Positi
26 October, 20212553 DownloadsNew Dental Implant Terminology for Exposing and Mitigating the Root Causes of Installation Related Treatment Complications
As knowledge about dental implant treatment increa
25 August, 20211611 DownloadsThe Screw versus Cement Debate: Will that be Peri-implant Disease by Misfits and Poor Access to Care or Bad Margins and Subgingival Cement?
Will that be Peri-implant Disease by Misfits and P
23 August, 2021756 Downloads
Why and When does Splinting Crowns and Bridges make Treatment Better for Patients
Abstract: In Spectrum Implants October 2022 I intr
03 February, 2023893 DownloadsThe Reverse Margin System and Supporting Concepts Designed to Make Implant Treatment Better
Abstract: The Reverse Margin System (RMS) d
02 January, 20231020 DownloadsDo Dental Implants Fail 10 Times More than Natural Teeth? A Critical Review and Related Commentary
Overly grandiose and poorly substantiated titles r
18 October, 2022757 DownloadsDo dentists receive the support they need from educators, dental laboratories, implant manufacturers, implant sellers, and Government regulators to enable them to do a better job for their patients?
Abstract: This article reveals the perspective of
14 October, 2022534 DownloadsSafer Intraoral Cementation is the Gold Standard for Fixed Prostheses Installation
Abstract: This slide presentation is a concise ove
08 June, 2022661 DownloadsScrewmentation The Svoboda Way
Abstract: What prompted the development of the pro
02 June, 2022649 DownloadsEffect of Margin Design, its Subgingival Depth and Installation Pressure on Subgingival Cement and Open Margins: an in vitro study
Emil LA Svoboda PhD, DDS, Anit Sharma DDS a
23 May, 2022665 DownloadsThe Big Question with Emil Svoboda PHD DDS
I welcome all your questions and comments. I hope
25 April, 2022627 DownloadsFixed Prosthesis Installation: An Aviation Analogy Considering 3-D Position, Yaw, Pitch and Roll
Citation: Svoboda E.L.A. Fixed Prosthetics: Positi
26 October, 20212553 DownloadsNew Dental Implant Terminology for Exposing and Mitigating the Root Causes of Installation Related Treatment Complications
As knowledge about dental implant treatment increa
25 August, 20211611 DownloadsExploring the BIG QUESTIONS about Implant Dentistry
Welcome to my new feature, Exploring the BIG QUEST
23 August, 20211558 DownloadsThe Screw versus Cement Debate: Will that be Peri-implant Disease by Misfits and Poor Access to Care or Bad Margins and Subgingival Cement?
Will that be Peri-implant Disease by Misfits and P
23 August, 2021756 DownloadsComparing the Chamfer and Reverse Margin System at Preventing Submarginal Cement
Emil LA Svoboda PHD, DDS. Anit Sharma DDS, Majid Z
16 June, 20211204 DownloadsMisfit implant parts and poor margins are the Standard of Care for implant prosthetics. Is anyone conflicted about this?
Citation: Svoboda Emil LA. Misfit implant parts an
10 May, 20211169 DownloadsAll-On-X A New Standard of Care
Citation: Svoboda Emil LA. All-On-X A New Standard
01 May, 2021928 DownloadsSafer Implant Treatment: Mitigating the Root Causes of Complications Related to Current Prostheses Installation Techniques Dr. Emil Svoboda
Citation: Svoboda ELA. Safer Implant Treatment: Mi
19 April, 20211327 DownloadsDental Implant Prosthetics: Achieving Retrievability and Reducing Treatment Complications by using a Modified Installation Technique Dr. Emil Svoboda
Citation: Dental Implant Prosthetics: Achieving Re
10 April, 20212088 DownloadsPreventing Peri-implant Disease by Safer Prosthesis Installation: Managing the Macrogap and Residual Subgingival Cement
Dental implants are used in dentistry as tooth roo
25 March, 20211648 Downloads
Making the Screw-in Prosthesis Installation System Safer
Abstract: There is a growing concern regarding the
13 May, 20241015 DownloadsMaking Fixed Prosthesis Installation Safer by Preventing Several Risk factors for Peri-implant Disease
Abstract: There continues to be much dialogue abou
07 December, 2022603 DownloadsSafer Intraoral Cementation is the Gold Standard for Fixed Prostheses Installation
Abstract: This slide presentation is a concise ove
08 June, 2022661 DownloadsTaming the Old Dragons of Dental Implant Prosthetics Dr. Emil Svoboda
Citation: Svoboda Emil LA. Taming the OLD Dragons
05 June, 20191031 DownloadsScrew versus Cement for Implant Prosthesis Installation. Part 2: The Game Changer the Tips the Balance to Favour Intra-oral Cementation
Part 2 [slideshare [slideshare id=56838352&
02 January, 2016Screw Vs Cement for Dental Implant Prosthesis Installation Part 1: The Logic Behind the Argument Dr. Emil Svoboda
Part 1 Screw Vs Cement for Dental Implant P
02 January, 2016